Researchers from Amsterdam UMC and UMC Utrecht developed a multifaceted intervention to improve the recognition and treatment of urinary tract infections in frail older adults. Use of this intervention resulted in a more than 50 percent reduction in antibiotic use for urinary tract infections, without evidence of negative effects. These were the most important findings of the thesis of Esther Hartman, who defends her PhD thesis in Amsterdam this week.
Physicians frequently prescribe antibiotics for a suspected urinary tract infection in frail older adults. Some of these antibiotics prescriptions are not necessary. Recognition and diagnosis of urinary tract infections is often difficult. Sometimes, health care professionals mistakenly suspect a urinary tract infection in case of only non-specific symptoms such as smelly urine or a change in behaviour. Furthermore, frail older adults frequently have bacteria in the urine without a urinary tract infection. If the urine test is positive, this is often misinterpreted as a urinary tract infection, leading to an antibiotic prescription. As a result, older adults are unnecessarily exposed to side effects. Moreover, antibiotic overuse can lead to antimicrobial resistance, which happens when bacteria no longer respond to antibiotics. In that case, infections cannot be treated.
Guidelines recommend using antibiotics only when necessary, in case of symptoms that are specific for urinary tract infections. In practice, these recommendations can be difficult to follow. We aimed to improve antibiotic prescribing for urinary tract infections in frail older adults, and performed an international study at the department of Medicine for Older Adults, Amsterdam UMC and the department of General Practice & Nursing Science of the Julius Center, UMC Utrecht.
The study took place in general practices and older adult care organisations in the Netherlands, Norway, Sweden, and Poland. The researchers interviewed older adults, caregivers, nurse assistants, nurses and general practitioners. These interviews helped to better understand the process leading to the decision to prescribe antibiotics or not. The study shows that this decision is often complex. Many different people can be involved, including the older patient, caregivers, nurse assistants, nurses, general practice assistants and physicians. Also, many factors influence the decision, such as knowledge of health care professionals, communication, and organisation of care.
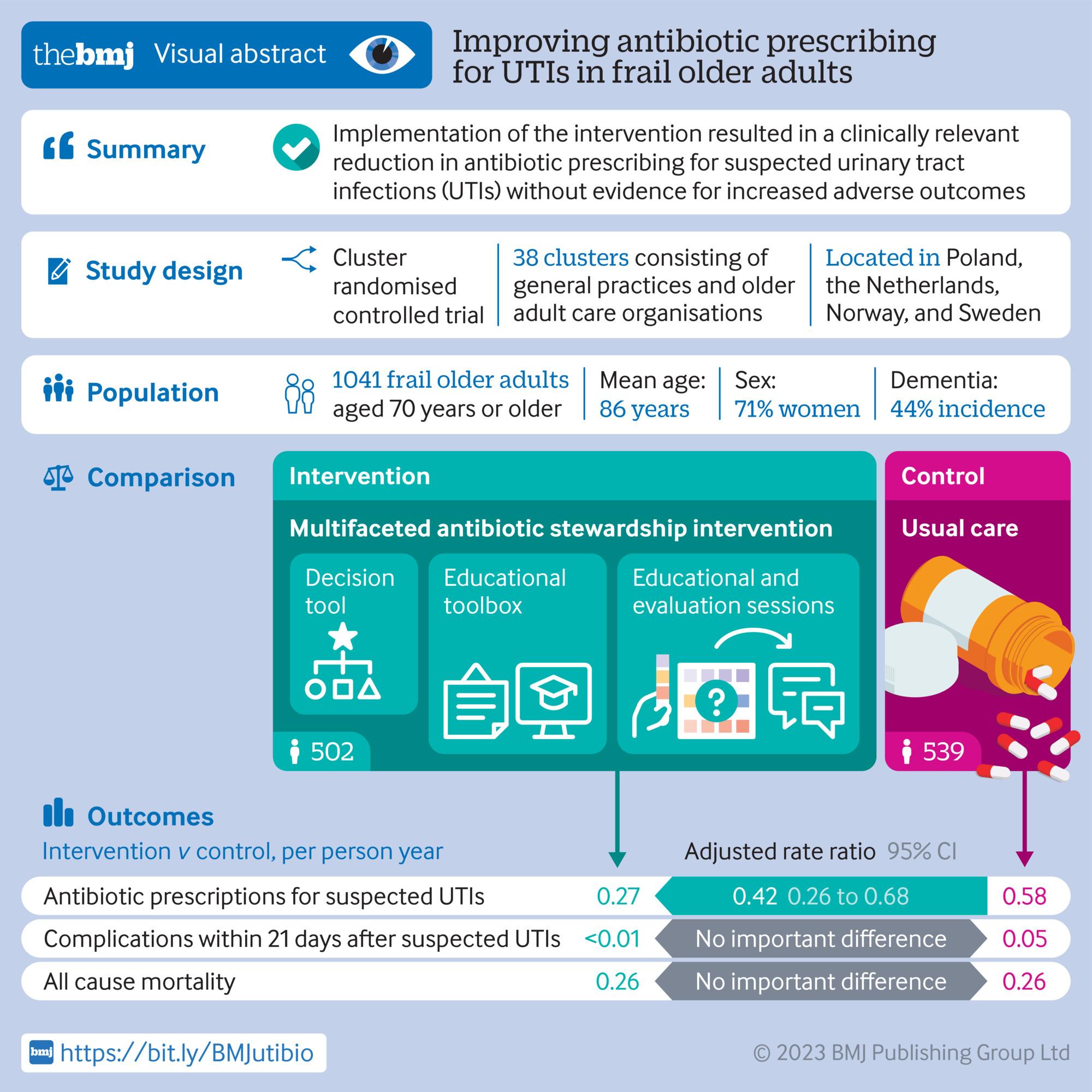
Next, the researchers developed a multifaceted intervention to improve the recognition and treatment of urinary tract infections. It consists of a decision-tool, supportive materials, educational and evaluation sessions. The intervention is in line with current guidelines. Esther Hartman (Amsterdam UMC), who defends her PhD thesis this week, says: “We performed a cluster-randomised trial to evaluate the intervention, with data from over a 1000 frail older adults. After randomisation, half of participating organisations received the intervention. The other half performed care as usual. We found that the multifaceted intervention is effective in reducing antibiotic use for suspected urinary tract infections, without evidence for negative outcomes.”
Currently, a follow-up study is ongoing to scale up the intervention for use in clinical practice in the Netherlands. In time, the researchers hope that all general practitioners and health care professionals in older adult care will have access to the intervention.
Esther Hartman, MD MSc (1993, Hilversum) will defend her PhD thesis on April 4, 2025 at the Vrije Universiteit Amsterdam. The title of her thesis is “Improving antibiotic prescribing decisions on suspected urinary tract infections in frail older adults – A tailored approach in four European countries”. Supervisors are prof. Cees Hertogh, MD PhD (Department of Medicine for Older People, Amsterdam UMC) and prof. em. Theo Verheij, MD PhD (Department of General Practice & Nursing Science, UMC Utrecht). Co-supervisors are Wim Groen, MD, PhD (Department of Medicine for Older People, Amsterdam UMC) and Alma van de Pol, MD, PhD (Department of General Practice & Nursing Science, UMC Utrecht). Esther Harman combines her PhD with her specialization in older adult care medicine, which she expects to finish in June 2025.